Lisfranc injury treatment1/5/2024  After four to six weeks, patients can wear normal shoes, weight-bear as tolerated, and begin gentle range-of-movement exercises. immobilization in a boot, is advised for stable injuries, for example, partial sprains and extra-articular fractures. 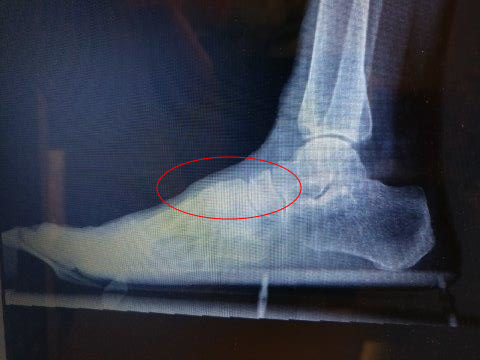
CT may be beneficial in assessing minor Lisfranc injuries, particularly for polytrauma patients or those unable to tolerate weight-bearing X-rays, and to demarcate proximal fracture line extension into the navicular, cuboid, or cuneiforms. Disturbance of the Lisfranc ligament complex is highly indicative of unstable foot injury. MRI is useful in detecting minor Lisfranc injuries and for those who are unable to tolerate weight-bearing X-rays. Disturbance of any of these anatomical relationships indicates Lisfranc injury. On a weight-bearing lateral view, the long axis of the talus should align with the medial and middle foot columns. The medial side of the cuboid should align with the medial side of the fourth metatarsal. On a weight-bearing oblique view, the medial side of the lateral cuneiform should align with the medial side of the third metatarsal. The medial side of the middle cuneiform should align with the medial side of the second metatarsal. On a weight-bearing anteroposterior view of the foot, the borders of the medial cuneiform should align with the borders of the first metatarsal. Fluoroscopic stress views are also helpful but they are painful and require anaesthesia. Weight-bearing X-rays and comparisons with the unaffected foot may help in diagnosing subtle injuries. Clinicians should be guided by the clinical picture even if X-rays are normal, as Lisfranc injuries are easily missed. Regarding imaging, an X-ray is used as a first-line with weight-bearing anteroposterior, oblique and lateral views. The midfoot will be tender on palpation and passive forefoot movement will elicit pain. Patients typically present in significant pain, unable to weight-bear, with midfoot swelling. A detailed history of the mode of injury is important including foot position, degree of energy involved, and force direction. Missed and delayed diagnoses are associated with devastating long-term disabilities. The incidence of missing a Lisfranc injury is 20% and typically occurs in low-energy injuries and polytrauma patients. Ī thorough history and examination are key in assessing Lisfranc injuries. The Lisfranc ligament is the most robust ligament, and the second metatarsal is important in stabilising the midfoot arch. The Lisfranc ligament complex encompasses the Lisfranc ligament and the first and second metatarsals’ TMT ligaments. Dorsal displacement in Lisfranc injuries occurs as the dorsal ligaments are weaker (ii) Inter-metatarsal ligaments, which connect the second to fifth metatarsals (iii) Lisfranc ligament, the plantar interosseous ligament connecting the medial aspect of the second metatarsal to the lateral aspect of the first cuneiform bone. Ligamentous structures are critical in stabilising the Lisfranc joint and comprise: (i) TMT plantar and dorsal ligaments, which cross every TMT joint. Studies show that a shallow second tarsometatarsal (TMT) joint mortise increases the risk of Lisfranc injury. Between the medial and lateral cuneiform lies the base of the second metatarsal. The bases of the metatarsals form an arch-like structure with the second metatarsal acting like a keystone. The osseous structure of the midfoot makes it inherently stable. The Lisfranc joint complex comprises the first to fifth metatarsals, three cuneiforms, the cuboid, communicating ligaments, capsules, and stabilising tendons. 
This review will focus on the current literature on Lisfranc injury management. Delayed or missed diagnoses are associated with arch collapse, midfoot instability, post-traumatic osteoarthritis, and forefoot abduction, which cause stiffness, chronic pain, and foot and ankle complex dysfunction. Studies report that 20% of Lisfranc injury diagnoses are missed initially, likely due to the intricate anatomy of the midfoot rendering diagnosis and detection of subtle cases difficult using X-ray alone. Lisfranc injuries can result from high-impact injuries sustained from motorcycle accidents or high velocity falls, or low-impact injuries sustained from sports. This term originates from Jaque Lisfrant de Saint-Martin, a French military surgeon and gynaecologist who described both the injury and amputation through the midfoot. Lisfranc injuries encompass bony or ligamentous injuries where one or more metatarsal is displaced relative to the tarsus. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
